Services
Assessment
A detailed, comprehensive assessment will be undertaken by your physiotherapist, involving history taking and physical examination. The assessment will ascertain:
- The current pathology.
- The probable cause of the condition.
- Contributing factors that may affect recovery.
After the assessment your physiotherapist will discuss with you the diagnosis, treatment required, expected outcome and indicate the likely number of sessions you require. If necessary a referral to an appropriate medical professional will be arranged for you.
Treatment
The second stage involves your treatment. Forde clinic approach to treatment is centred around manual therapy. Manual therapy involves the mobilisation and manipulation of joints, nerves and muscles.
This allows us to correct postural dysfunctions and movement abnormalities facilitating early healing. Your physiotherapist may ask you to maintain these corrections by performing simple exercises at home or work.
Rehabilitation & Prevention
The aim of this third and final stage is to prevent recurrence by addressing the contributing factors to your injury or condition. Your physical therapist will design a specific programme of exercises for you to improve muscle function and maximise your body's potential.
By completing this rehabilitation programme you will be encouraged towards independent self management of your condition.
Advice on training programmes and office ergonomics will be given by your physical therapist when appropriate.
Conditions Treated
We treat a wide range of conditions across all age groups. The following is just a brief overview of some of the conditions that we treat. If you are unsure as to whether your condition is treatable by us, please contact us.
-
Musculoskeletal Conditions
Musculoskeletal complaints include the muscles or associated soft tissues of the skeletal system such as tendons, ligaments and nerves.
Some common musculoskeletal conditions that we treat at the clinic include:
- Low back pain
- Neck pain
- Muscle Spasm
- Postural conditions
- Sciatica
- Whiplash
- Trapped Nerves
- Prolapsed discs
- Facet joint dysfunction
- Rotator Cuff injuries
- Cervicogenic Headaches
- Bursitis
- Carpal Tunnel Syndrome
- Impingement Syndromes
-
Sports Injuries
Some common sports injuries that we treat at the clinic include:
- Ankle sprains
- Hamstring strains and ruptures
- Achilles tendonitis
- Shin splints
- Stress Fractures
- Groin injuries
- Jumpers knee
- Osteitis pubis
- Dislocated shoulders
- ACL tears
- Meniscal injuries
- MCL/LCL tears
- Patellofemoral syndrome
- Tennis Elbow
- Bursitis
-
Biomechanical Conditions
Biomechanics refers to the analysis of human movement and how the human body is affected by external forces
Our physiotherapists are trained in biomechanical correction, that relate to mal-alignments throughout the body that can give rise to injuries such as:
- Foot Pain (e.g. Plantar fasciitis, heel pain, arch pain, metatarsalgia, bunions)
- Calf strains
- Shin splints
- Achilles tendonitis
- Knee pain
- Low back pain
Physiotherapy
Physiotherapy (also called physical therapy) is a healthcare profession that helps people restore movement, reduce pain, and improve physical function after injury, illness, surgery, or disability.
What Physiotherapy Helps With
Physiotherapy is commonly used for:
- Back and neck pain
- Sports injuries
- Joint problems (knee, shoulder, hip pain)
- Recovery after surgery
- Stroke rehabilitation
- Arthritis
- Muscle strains and sprains
- Posture problems

Therapeutic lasers are also effectively used on trigger points in musculoskeletal treatments and can provide drug-free pain relief, being of particular aid in the treatment of arthritic conditions and neuralgic pain
Low-Level Laser Therapy (LLLT)
Low-Level Laser Therapy (LLLT) — also called cold laser therapy or photobiomodulation (PBM) — is a non-invasive treatment that uses low-intensity light to stimulate healing and reduce pain.
Unlike surgical lasers, it does not cut or heat tissue. The energy level is low enough that you don’t feel burning.
-
Example applications for physical therapists are:
- Arthritic conditions
- Tendonitis
- Epicondilitis
- Carpel Tunnel Syndrome
- Neuralgic Pain
-
Arthritic Conditions
Laser therapy delivers pain-relief and addresses the inflammation in arthritic conditions.
With Rheumatoid arthritis, laser therapy influences small joints directly and large joints indirectly. It strengthens the antiphlogistic processes and depresses the autoimmune response. The effects in the early stages of the condition can be impressive, but with chronic conditions, although pain is eased on treatment, longer treatment courses measured in months are necessary in order to make a substantive differences to the condition. It has been reported that 6 months can be a turning point. It also appears that adding laser therapy to prescribed medication gives improved results over medication alone.
With gout, attacks can be curtailed and the symptoms reduced. Laser therapy inhibits inflammation, eases pain, reduces swelling and joint tenderness.
In cases of osteoarthritis, laser therapy may slow down the degenerative process as well as ease acute symptoms. In the case of large joints such as the hip joint, the therapeutic effects of laser are brought on by an improvement and strengthening of the surrounding tissues. Laser therapy activates the microcirculation and the metabolism, prevents oedema and triggers anti-inflammatory processes in the synovial membrane.
-
Clinical Applications Overview
Laser therapy is effective across a wide range of conditions and therefore used in a variety of health care and veterinary disciplines. There is consequently a large body of research to be found on the clinical effects of low level laser both in vitro and in vivo. This is spread across many fields and many nations, with work from Russia, Israel, Italy, Spain Japan, Denmark and Australia amongst others.
In the UK, a large volume of controlled research has been carried out in centres of excellence such as Guy's Hospital Tissue Repair Unit, Oxford University, Ulster University, Cambridge Military Hospitaland Northampton School of Podiatry.
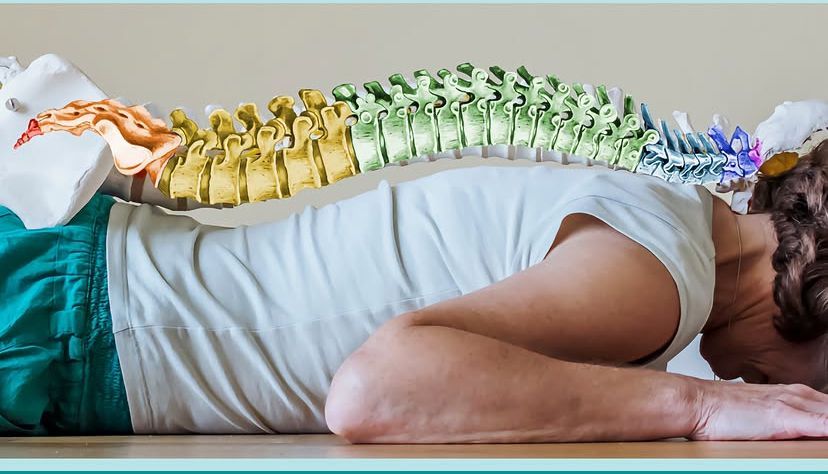
Spinal Decompression Therapy
Spinal decompression therapy is a non-surgical treatment designed to relieve back and neck pain by gently stretching the spine in a controlled way. It’s most often used for problems involving spinal discs and nerve compression.
-
What Does Spinal Decompression Treat?
It’s commonly used for:
- Herniated or Bulging Discs: When a spinal disc pushes out of place and presses on a nerve.
- Degenerative Disc Disease: Age-related disc wear and tear that causes pain and stiffness.
- Sciatica: Pain that radiates down the leg due to compression of the sciatic nerve.
- Spinal Stenosis: Narrowing of the spinal canal that compresses nerves.
- Facet Joint Syndrome: Irritation of the joints connecting the vertebrae.
- Chronic Lower Back or Neck Pain: Especially pain that hasn’t improved with rest, medication, or physical therapy.
-
How Does It Work?
Spinal decompression is usually done using a motorized traction table.
Step-by-step process:
1. You lie on a specialized table.
2. A harness is placed around your hips (for low back) or neck (for cervical spine).
3. The machine gently stretches and relaxes the spine in cycles.
4. This creates negative pressure inside the discs.
What that negative pressure does:
• Pulls herniated or bulging disc material back inward
• Reduces pressure on nerves
• Improves blood flow and nutrient exchange to damaged discs
• Helps promote healing
Think of it like creating a slight “vacuum effect” inside the disc.
-
What It Feels Like
Most people describe it as:
- A gentle pulling sensation
- Relaxing rather than painful
- Sessions typically last 20–45 minutes
- A treatment plan often involves multiple sessions over several weeks
-
Is It Effective?
Some people report significant relief, especially for disc-related nerve pain. However:
• Research results are mixed
• It tends to work best when combined with physical therapy and strengthening exercises
• It may not help structural problems that require surgery
Emsella Treatment Chair
Emsella is a non-invasive treatment designed to strengthen the pelvic floor muscles. It uses high-intensity focused electromagnetic (HIFEM) technology to cause thousands of supramaximal muscle contractions in a single session — much stronger than what you can do with voluntary Kegels.
You sit fully clothed on a specialized chair, and the device stimulates the pelvic floor muscles without probes or surgery.
-
What Does It Treat?
1. Urinary Incontinence (Most Common Use)
Especially:
• Stress incontinence (leaking when coughing, laughing, exercising)
• Urge incontinence (sudden strong urge to urinate)
• Mild to moderate mixed incontinence
2. Postpartum Pelvic Floor Weakness
After pregnancy and childbirth.
3. Age-Related Pelvic Floor Weakness
Common in women over 40, but men can also benefit.
4. Erectile Dysfunction (in Men)
Some clinics use it to improve pelvic muscle strength that supports erections.
5. Post-Prostate Surgery Incontinence
Helps men regain bladder control.
-
How Does It Work?
The device generates focused electromagnetic energy that:
1. Penetrates deep into pelvic muscles.
2. Causes rapid involuntary contractions.
3. Strengthens and re-educates weak muscles.
4. Improves neuromuscular control.
One 28-minute session is often said to equal ~11,000 Kegel contractions.
Over several sessions (commonly 6–8 treatments):
• Muscle tone improves
• Bladder support increases
• Leakage episodes often decrease
-
What It Feels Like
- A tingling or tapping sensation
- Strong pelvic muscle tightening
- No pain for most people
- No downtime — you can resume normal activity immediately
-
Who It’s Not For
It’s generally avoided in people with:
• Metal implants in the pelvic area
• Pacemakers or implanted defibrillators
• Active pregnancy
• Certain neurological conditions
-
Is It Effective?
Studies and clinical reports show:
- Many patients see noticeable improvement after a full treatment series
- Results vary
- Maintenance sessions are sometimes needed
It works best for mild to moderate symptoms. Severe pelvic organ prolapse or advanced incontinence may require other treatments.
Gait & Foot Scan
A gait analysis and foot scan evaluates how you walk or run and how your feet function under load. It’s commonly performed in podiatry, sports medicine, chiropractic, and physical therapy clinics to diagnose biomechanical issues and design custom orthotics.
The TOG GaitScan™ is an innovative diagnostic tool and digital casting device that allows practitioners to analyze patient biomechanics and order custom orthotic products. With 4096 sensors and a scan rate of 300 frames per second, GaitScan™ is the industry leader in dynamic scanning capabilities.
What does this mean for you? A new, in-depth method of assessing your gait cycle with a dynamic scan gives your health care provider access to a wealth of information that cannot be obtained with the naked eye. Over a million points of data are recorded, tracking minor flaws in your biomechanics and shedding light on issues that if left untreated, could develop into painful conditions over time.
The TOG GaitScan™ is a valuable education tool that provides practitioners with a comprehensive biomechanical analysis for each patient as well as clear, concise images to assess and articulate the need for orthotic therapy.
-
What Is Gait Analysis?
Gait analysis studies:
- How your foot strikes the ground (heel, midfoot, forefoot)
• Pronation or supination (how much your foot rolls inward/outward)
• Step length and symmetry
• Hip, knee, and ankle alignment
• Weight distribution during movement
Tools Used:
• Video analysis (sometimes slow-motion)
• Pressure plates or treadmill sensors
• Motion capture systems
• Clinical orthopedic tests
-
What Is a Foot Scan?
A foot scan captures the shape and pressure pattern of your feet.
Types of Scans:
1. Static scan – Standing still to see arch height and pressure points.
2. Dynamic scan – Walking across a pressure plate to measure force and balance.
3. 3D digital scan – Creates a detailed model of your foot for orthotic design.
The scan shows:
• Arch type (low, normal, high)
• Pressure hotspots
• Asymmetries between left and right foot
• Areas prone to overuse injuries
-
Conditions It Helps Identify
• Plantar fasciitis
• Flat feet (pes planus)
• High arches (pes cavus)
• Overpronation / oversupination
• Heel pain
• Shin splints
• Knee, hip, or lower back pain related to foot mechanics
• Diabetic pressure risk areas
-
Orthotic Production — How Custom Inserts Are Made
Once your gait and scan data are collected, custom orthotics are designed to correct or support your biomechanics.
Step-by-Step Process:
1. Data Collection
Foot scan + gait analysis + clinical exam.
2. Prescription Design
Clinician determines:
◦ Arch support level
◦ Heel posting (tilt correction)
◦ Cushioning material
◦ Rigidity vs flexibility
◦ Shock absorption needs
3. Digital Modeling
Software adjusts the 3D foot model to correct alignment.
4. Manufacturing
◦ 3D printing
◦ CNC milling
◦ Layered foam/composite molding
5. Fitting Appointment
Orthotics are adjusted for comfort and shoe fit.
-
What Orthotics Actually Do
They can:
• Redistribute pressure
• Reduce excessive pronation
• Improve alignment of ankle, knee, and hip
• Decrease strain on plantar fascia
• Improve shock absorption
• Reduce fatigue during standing or walking
They do not permanently “fix” foot structure, but they support better mechanics while worn.
-
Who Benefits Most?
• Runners or athletes
• People who stand all day
• Chronic heel or arch pain sufferers
• Flat feet with knee or back pain
• Diabetics needing pressure offloading
• Post-injury rehabilitation patients
-
Important Note
Custom orthotics are different from:
• Over-the-counter inserts (generic support)
• Shoe store pressure scans (screening, not medical evaluation)
Medical-grade orthotics are prescribed based on clinical findings, not just arch shape.
-
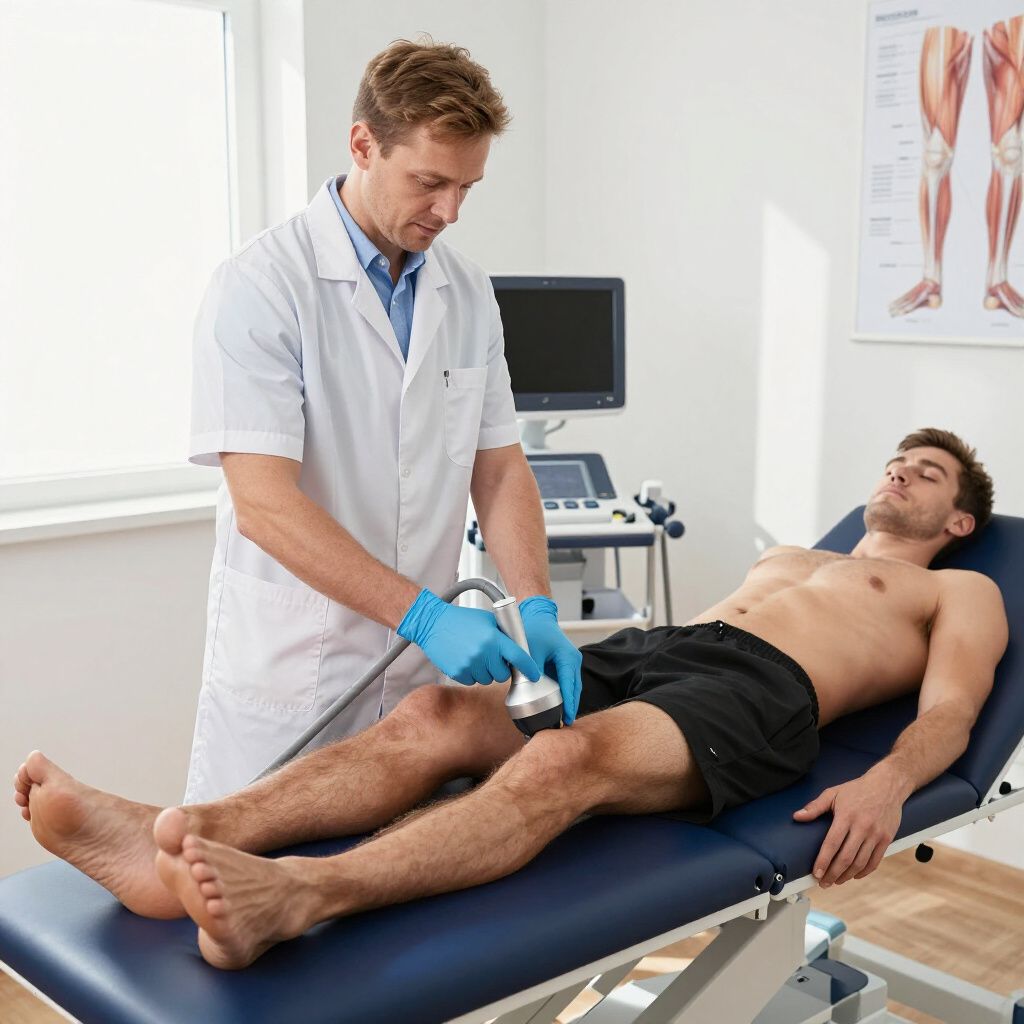
What is Shockwave Therapy
Shockwave therapy (Extracorporeal Shockwave Therapy, ESWT) is a non-surgical treatment that uses high-energy sound waves to stimulate healing in injured tissues.
It’s most commonly used for chronic tendon and soft-tissue conditions, especially when pain has lasted more than a few months and hasn’t improved with rest, physical therapy, or medication.
-
What Shockwave Therapy Treats
Foot & Ankle
Plantar fasciitis (chronic heel pain)
Achilles tendinopathy
Heel spurs
Elbow
Tennis elbow (lateral epicondylitis)
Golfer’s elbow (medial epicondylitis)
Knee
Patellar tendinopathy (jumper’s knee)
Shoulder
Calcific tendinitis (calcium deposits in the rotator cuff)
Chronic rotator cuff tendinopathy
Hip
Greater trochanteric pain syndrome (gluteal tendinopathy)
Muscle Pain
Myofascial trigger points
Chronic muscle tightness
-
How Low-Level Laser Therapy (LLLT) Works
LLLT uses specific wavelengths of red or near-infrared light that penetrate the skin and are absorbed by cells. This can:
• Increase cellular energy (ATP production)
• Improve blood flow
• Reduce inflammation
• Accelerate tissue repair
• Decrease pain signals
The light stimulates mitochondria (the “energy factories” of cells), helping damaged tissue heal more efficiently.
LLLT is used for:
• Tendonitis and ligament injuries
• Neck and back pain
• Arthritis
• Muscle strains
• Nerve pain
• Wound healing
• Sports injuries
• TMJ pain
• Hair loss (in specific FDA-cleared devices)
Shockwave Therapy
Shockwave therapy (Extracorporeal Shockwave Therapy, ESWT) is a non-surgical treatment that uses high-energy sound waves to stimulate healing in injured tissues.
It’s most commonly used for chronic tendon and soft-tissue conditions, especially when pain has lasted more than a few months and hasn’t improved with rest, physical therapy, or medication.
You Don’t Have to Live With Pain
Whether your pain is recent or long-standing, we’re here to help you restore movement, reduce discomfort, and regain your quality of life.